At least one new HIV case has been linked to vampire facials performed at the VIP Beauty Salon and Spa in Albuquerque, which closed nearly five years ago, according to a press release from the New Mexico Department of Health. In 2019, two other HIV cases were traced to the spa.
Once again, health officials urge former clients to get tested for HIV and hepatitis B and C. “It’s very important that we spread the word and remind people who received any kind of injection-related services provided at the VIP Spa to come in for free and confidential testing,” said Laura Parajon, MD, MPH, the deputy secretary for the health department, in the press release.
In the statement, the health department said it “has reopened the investigation. As of July 5, 2023, [the health department] has identified additional HIV infections with direct or indirect connection with services provided at the VIP Spa.”
No further information was available about those other cases.
The spa was closed in September 2018 after it was determined that some of its practices could have led to the spread of diseases, such as HIV, hepatitis B and hepatitis C, according to a 2019 press release from the health officials.
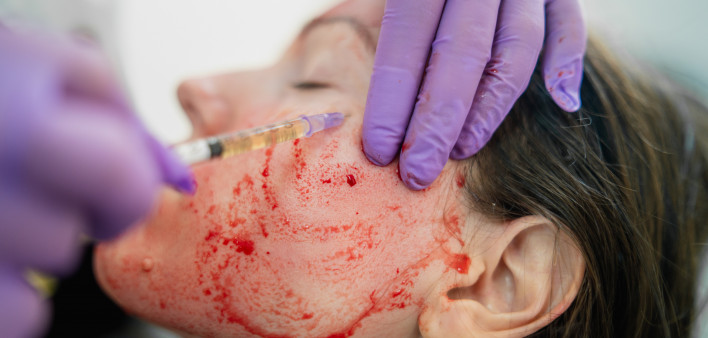
A vampire facial is a cosmetic procedure that involves injecting nutrient-rich plasma into the skin on the face to achieve a more youthful appearance. The plasma typically comes from an individual’s own blood.
When the procedure is carried out properly, it shouldn’t expose anyone to HIV, hepatitis or other blood-borne diseases. But if the equipment used during the procedure, such as a micro-needling pen, is not disposed of correctly or sterilized between facials, the risk of exposure to such diseases is high.
It’s estimated that about 1.2 million Americans are living with HIV and that 2.4 million Americans were living with chronic hep C between 2013 and 2016 (about 1% of the adult population), according to the Centers for Disease Control and Prevention. What’s more, 14,242 people died of hepatitis C in 2019, and acute hep C cases quadrupled from 2009 to 2019. Nearly 862,000 were living with chronic hep B in 2019. These numbers are likely higher now, spurred by the opioid crisis.
Hepatitis refers to inflammation of the liver. When untreated, it can lead to scarring of the liver (cirrhosis), liver cancer, the need for a liver transplant and death. Hepatitis can be caused by several factors, including toxins, excess alcohol use, autoimmune diseases, fat in the liver and viruses, including the three most common ones: hepatitis A, B and C. (Hep A is transmitted through contaminated food and water.) Effective vaccines are available for hep A and B. What’s more, hep C (but not HIV and hep B) is curable in most cases.
According to “Hepatitis C Transmission and Risk,” part of Hep’s Basics of Hepatitis, hep C is most easily spread through:
- Sharing needles and other equipment (paraphernalia) used to inject drugs;
- Blood transfusions and organ transplants before July 1992;
- Sexual contact with someone who has hep C;
- Having a mother who had hep C when you were born.
HIV, in contrast, is a virus that attacks the immune system. Over several years, the immune system becomes depleted, and the body isn’t able to fight infections, leading to an AIDS diagnosis.
Although there is no cure for HIV, many safe and effective treatments—often just one pill a day—are available. The medications help people living with HIV enjoy long and healthy lives and keep them from transmitting the virus to others. For more, see the Basics of HIV/AIDS in POZ.com, a sister publication of HepMag.com, RealHealthMag.com, CancerHealth.com and TuSaludMag.com.
According to HIV Transmission and Risks in the POZ Basics: HIV is transmitted through the following body fluids:
- Blood
- Semen
- Pre-cum
- Rectal fluids
- Vaginal fluids
- Breast milk.
There are several ways this can happen:
- From condomless vaginal/frontal or anal sex with someone who has HIV while not using a condom or not using medicines to prevent (pre-exposure prophylaxis [PrEP] or post-exposure prophylaxis [PEP]) or treat HIV (Undetectable Equals Untransmittable, or U=U).
- From sharing needles, syringes or other injection equipment with someone who has HIV while not using PrEP.
- From mother to child during pregnancy, childbirth or breastfeeding. However, if the mother is in regular care and on HIV treatment, this risk is reduced to nearly zero.
- From being stuck with a needle or cut with a sharp object that contains HIV-positive blood. This is mostly a risk for health care workers.
- From getting a blood transfusion. However, this risk is rare in United States.
HIV is not transmitted though saliva, urine, feces, vomit, sweat, animals, bugs or the air.






Comments
Comments